.png)
Monkeypox (Mpox) is an infectious disease spread through close contact with contagious individuals or infected animals. Most people recover fully, but in some cases, it can lead to severe illness or death.
Vaccination against smallpox offers some degree of protection against monkeypox. Smallpox was eradicated in 1980, so vaccination rates against it have dropped since then. This means the protection it provided against monkeypox has diminished, leading to a gradual increase in cases in West and Central Africa.
In 2022, an outbreak occurred Europe and spread globally, in which the disease was transmitted between humans, mainly through sexual contact, although this type of transmission is not the most common form of transmission. Since 2023, an epidemic of a new variant of monkeypox, known as clade 1b, began in Central Africa. In August 2024, the WHO declared this new monkeypox outbreak a public health emergency of international concern.
Monkeypox is a rare disease caused by the monkeypox virus that is usually transmitted from animals to humans. The disease is caused by the Monkeypox Virus (MPXV), which is present in the wildlife (in certain small mammals). Monkeypox can spread between people, mainly through close contact, and occasionally from the environment to people via things and surfaces that have been touched by a person with monkeypox. In settings where the monkeypox virus is present among some wild animals, it can also be transmitted from infected animals to people who have contact with them.
Monkeypox usually occurs in Central and West Africa. Cases outside of Africa are often due to: international travel, imported animals, close contact with an animal or person with monkeypox.
Monkeypox spreads from person to person mainly through close contact with someone who has mpox. Close contact includes skin-to-skin and mouth-to-mouth, or mouth-to-skin contact, and can also include being face-to-face with someone who has mpox (such as talking or breathing close to one another, which can generate infectious respiratory particles). During the global outbreak that began in 2022, the virus mostly spread through sexual contact.
People with mpox are considered infectious until all their lesions have crusted over, the scabs have fallen off and a new layer of skin has formed underneath, and all the lesions in the body (in the mouth, throat, eyes, vagina and anus) have healed too, which usually takes from 2 to 4 weeks.
It is also possible for the virus to persist for some time on clothing, bedding, towels, electronics and surfaces that have been touched by a person with mpox. Someone else who touches these items may become infected, particularly if they have any cuts or abrasions or touch their eyes, nose, mouth or other mucous membranes without first washing their hands. Cleaning and disinfecting surfaces/objects and cleaning your hands after touching surfaces/objects that may be contaminated can help prevent this type of transmission.
The virus can also spread during pregnancy to the fetus, during or after birth through skin-to-skin contact, or from a parent with mpox to an infant or child during close contact.
Although getting mpox from someone who is asymptomatic (not showing symptoms) has been reported, there is still limited information on whether the virus can be transmitted from someone with the virus before they get symptoms or after their lesions have healed.
b. From Animals to Humans
Someone who comes into physical contact with an animal which carries the virus, such as some species of monkeys or a terrestrial rodent (such as the tree squirrel) may also develop mpox. Exposure by such physical contact with an animal or meat can occur through bites or scratches, or during activities such as hunting, skinning, trapping or preparing a meal. The virus can also be caught through eating contaminated meat which is not cooked thoroughly.
c. From Humans to Animals
There have been a few reports of the virus being identified in pet dogs. However, it has not been confirmed whether these were true infections or whether the detection of virus was related to surface contamination.
Since many species of animals are known to be susceptible to the virus, there is the potential for spillback of the virus from humans to animals in different settings. People who have confirmed or suspected mpox should avoid close physical contact with animals, including pets (such as cats, dogs, hamsters, gerbils), livestock and wildlife.
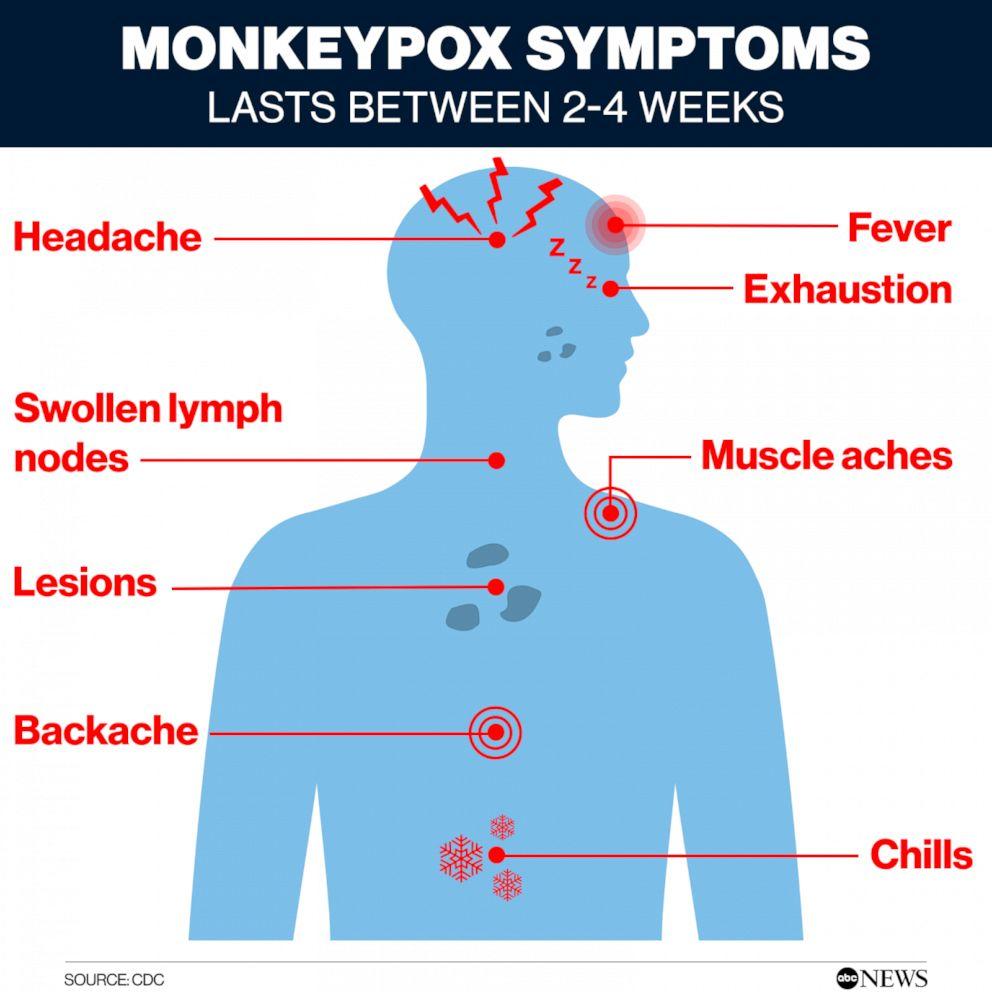
Mpox can cause a range of signs and symptoms. While some people have less severe symptoms, others may develop more serious illness and need care in a health facility. Mpox symptoms may start 3 to 17 days after you’re exposed and when you have symptoms is called the incubation period.
Common symptoms of mpox include a rash which may last for 2-4 weeks. This start with, or be followed by:
The rash looks like blisters or sores, and can affect the face, palms of the hand, soles of the feet, groin, gential and/or anal regions. These lesions may also be found in the mouth, throat, or on the eyes. The number of sores can range from one to several thousand. Some people develop inflammation inside the rectum (proctitis) that can cause severe pain, as well as inflammation of the genitals that may cause difficulties urinating.
In most cases, the symptoms of mpox go away on their own within a few weeks with supportive care, such as medication for pain or fever. However, in some people, the illness can be severe or lead to complications and even death. Newborn babies, children, people who are pregnant and people with underlying immune deficiencies such as from advanced HIV disease may be at higher risk of more serious mpox disease and death.
Complications can include severe bacterial infection from skin lesions, mpox affecting the brain (encephalitis), heart (myocarditis) or lungs (pneumonia), and eye problems. People with severe mpox may require hospitalization, supportive care and antiviral medicines to reduce the severity of lesions and shorten time to recovery.
The severity of the disease can vary depending on several factors including how the virus is transmitted, how susceptible the person is to the virus, and how much of the virus a person is exposed to. Complications of mpox in areas where it is most common include:
The mortality rate of mpox ranges from 0-11% in outbreaks, with young children being the most affected. Immunocompromised individuals are at a higher risk of severe disease and HIV-positive patients may experience more severe symptoms.
Most people with mpox will recover within 2-4 weeks. Things to do to help the symptoms and prevent transmitting mpox to others:
Do
Do not
To prevent spread of mpox to others, people with mpox should isolate at home following guidance from their health care provider, or in hospital if needed, for the duration of the infectious period (from onset of symptoms until lesions have healed and scabs fall off). Covering lesions and wearing a well-fitting mask when in the presence of others may help prevent spread. Using condoms during sex will help reduce the risk of getting mpox but will not prevent spread from skin-to-skin or mouth-to-skin contact.
Enhancing the immune system can be one of the measures taken to prevent someone from infecting by monkeypox. One of the components in supplements commonly used to boost the immune system is Echinacea and Black Elderberry.
Echinacea or cone flower is a flowering plant from Asteraceae family. Echinacea purpurea is one of the most widely used species for immunodulator. Based on research by Manayi, et. al. said that Echinacea purpurea has immunodulatory effects by increased activity of the body’s immune system such as neutrophils, macrophages, polymorphonuclear leukocytes (PMN) and Natural Killer cells (NK). Based on research by Dapas, et.al. Echinacea also has anti-inflammatory properties, with down-regulating IL-6 as inflammatory marker.
Based on Wasielica, et.al. Black Elderberry extract also found to alleviate the inflammatory response in activated RAW 264.7 macrophages by down-regulating the expression of pro inflammatory genes (TNF-α, IL-6, COX-2, iNOS) and suppressing the enhanced production of inflammatory mediators (TNF-α, IL-6, PGE2, NO).
Zinc picolinate and Selenium will increase the activity of immunodulator immune system so that is suitable to be used for prevention of disease.
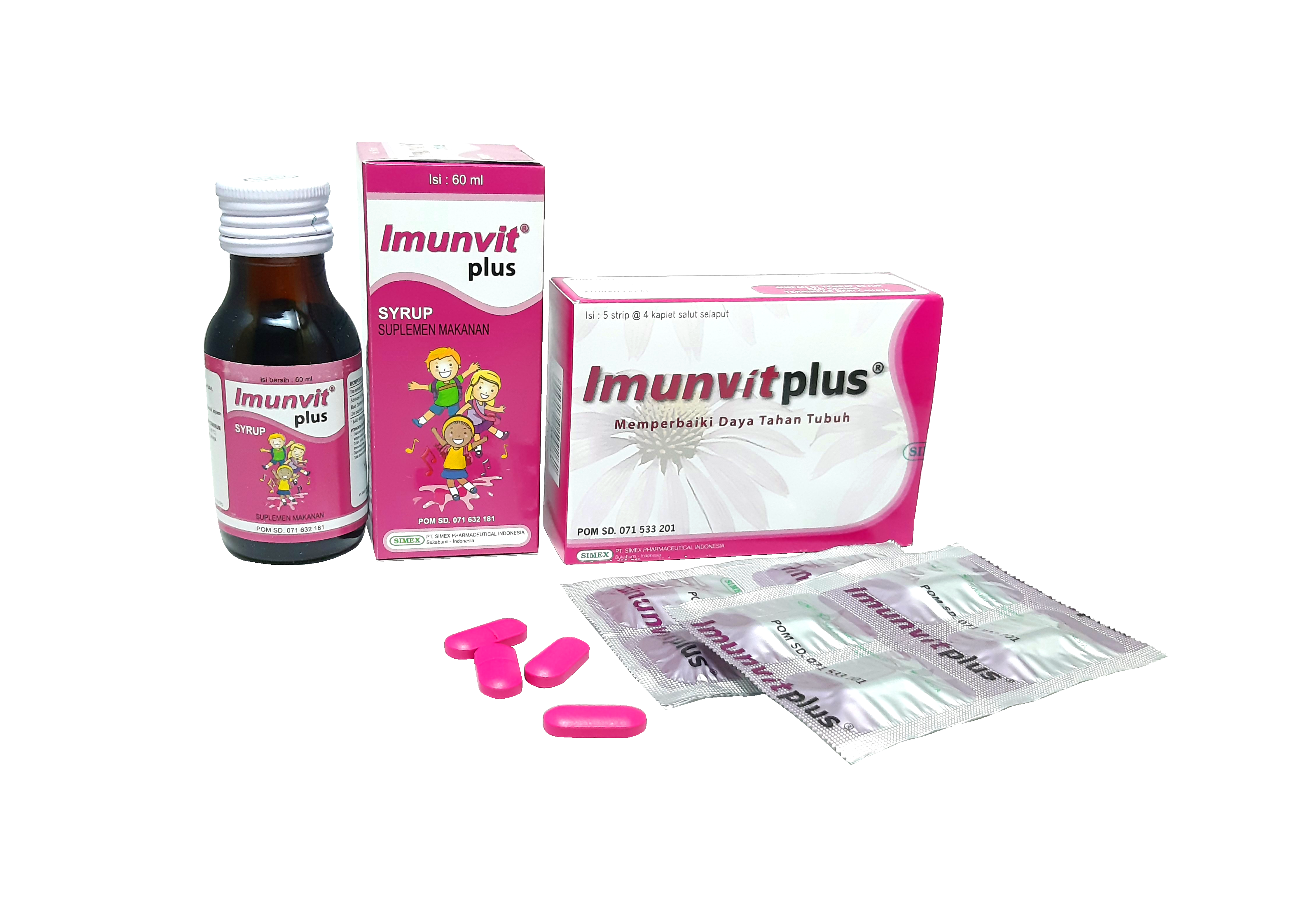
We can strengthen our immune system with immunodulatory supplements such as IMUNVIT PLUS® from PT Simex Pharmaceutical Indonesia. IMUNVIT PLUS® contains Echinacea, Black Elderberry, Zinc picolinate, and Selenium.
Many years of research on therapeutics for smallpox have led to the development of products that may also be useful for treating mpox. For example, an antiviral developed to treat smallpox (tecovirimat) was approved in January 2022 by the European Medicines Agency for the treatment of mpox under exceptional circumstances. Experience with these therapeutics in the context of an outbreak of mpox is growing but still limited. For this reason, their use is usually accompanied by enrolment in a clinical trial or expanded access protocol accompanied by the collection of information that will improve knowledge on how best to use them in future.
Getting a mpox vaccine can help prevent infection (pre-exposure prophylaxis), it is recommended for people at high-risk of getting mpox. At present, WHO recommends use of MVA-BN or LC16 vaccines, or the ACAM2000 vaccine when the others are not available. Only people who are at risk (for example, someone who has been a close contact of someone who has mpox, or someone who belongs to a group at high risk of exposure to mpox) should be considered for vaccination. Mass vaccination is not currently recommended. Travellers who may be at risk based on an individual risk assessment with their health care provider may wish to consider vaccination.
Group that may be at high risk of mpox include:
The vaccine can also be administered after a person has been in contact with someone who has mpox (post-exposure prohylaxis. In these cases, the vaccine should be given less than 4 days after contact with someone who has mpox. The vaccine can be given for up to 14 days if the person has not developed symptoms.
Some antivirals have received emergency use authorization in some countries and are being evaluated in clinical trials. To date, there is no proven effective antiviral treatment for mpox. Inosine pranobex (IP) as immunomodulatory agent maybe can help to attack monkeypox virus.
For decades now, IP has been a widely used drug due to its immunomodulatory and antiviral properties, and several mechanism of action have ben postulated in an effort to explain these properties. Studies have shown that IP can impact both the humoral as well as the cell-mediated aspects of the immune system, in such a way that it enhances the host immune responses and can also exhibit antiviral effects considerer secondary to this immunopotentiation.
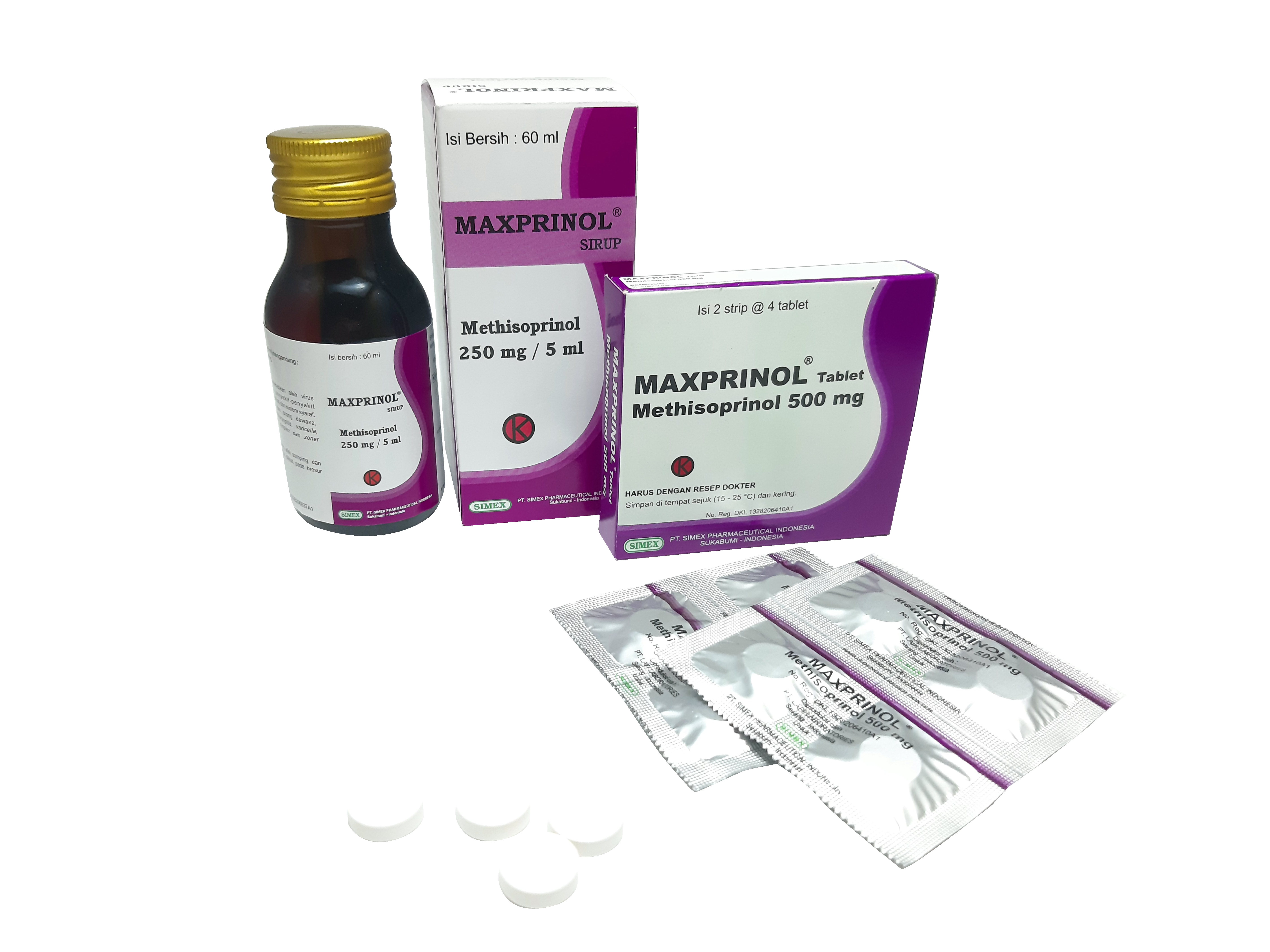
MAXPRINOL® from PT Simex Pharmaceutical Indonesia which contains Inosine Pranobex or Methisoprinol as immunomodulatory and antiviral properties to help against monkeypox virus.
Reference
https://ourworldindata.org/mpox
https://www.nhs.uk/conditions/mpox/
https://www.ecdc.europa.eu/en/mpox
https://www.who.int/news-room/questions-and-answers/item/mpox
https://abcnews.go.com/Health/symptoms-monkeypox-treat/story?id=84907957
Manayi A., Vazirian M., Seidnia S. 2015. Echinacea purpurea: Pharmacology, phytochemistry and analysis methods. Pharmacognosy Reviews. 2015; 9(17): 63-72
Dapas B., Dall'Acqua S., et.al. 2014. Immunomodulation mediated by a herbal syrup containing a standardized Echinacea root extract: A pilot study in healthy human subjects on cytokine gene expression. Elsevier: Phytomedicine 2014
Wasielica JZ., Olejnik A., et.al. 2019. Elderberry (Sambucus nigra L.) Fruit Extract Alleviates Oxidative Stress, Insulin Resistance, and Inflammation in Hypertrophied 3T3-L1 Adipocytes and Activated RAW 264.7 Macrophages. Foods 2019, 8, 326.
Silva J., Pantzartzi CN., Votava M. 2019. Inosine Pranobex: A Key Player in the Game Againt a Wide Range of Viral Infections and Non-Infectious Disease. Adv Ther