Allergic rhinitis (AR) is a growing global health issue. Globally, the prevalence of AR remains increasing, particularly in low- and middle-income countries, and ranges from 1.0% to 54.5%. The prevalence of AR is roughly 5% in children by 3 years of age, increases with age from 8.5% of 6–7 year-olds to 14.6% of 13–14 year-olds, and reaches more than 11.8% to 46% in people aged 20–44. Notably, the incidence of AR is higher in males than in females before puberty, but this trend reverses after puberty.
In Indonesia, the prevalence of allergic rhinitis is estimated to be 1.5-12.4% and tends to increase every year. According to several Indonesian studies, allergic rhinitis prevalence in children aged 13-14 was 16.4% in West Jakarta. It affects one in six individuals and is associated with significant morbidity, loss of productivity, and healthcare costs. Common allergic rhinitis complications include Sinusitis, nasal polyps, bronchial asthma, and otitis media.
Epidemiologically, AR affects 10–30% of world population and the prevalence is still increasing. According to the 2008 World Allergy Report, the prevalence of AR in the low and middle income countries within Asia Pacific Region was estimated to be around 5–45%.
Allergic rhinitis is an allergic reaction to tiny particles in the air called allergens. When you breathe in allergens through the nose or mouth, the body reacts by releasing a natural chemical called histamine. Frequent allergens include pollens, moulds, animal dander, and dust mites. The AR is characterized by rhinorrhea (watery runny nose), sneezing (especially violent and in bouts), nasal obstruction, itchy nose, and usually associated with eye symptoms.
Etiology of Allergic Rhinitis
The allergic response is classified into early and late-phase reactions. In the early phase, allergic rhinitis is an immunoglobulin (Ig) E – mediated response against inhaled allergen that cause inflammation. The initial response occurs within 5 to 15 minutes of exposure to an antigen, resulting in the degranulation of host mast cells. This releases a variety of pre-formed and newly synthesized mediators, including histamine, which is one of the primary mediators of allergic rhinitis. Histamine induces sneezing via the trigeminal nerve and also plays a role in rhinorrhea by stimulating mucous glands. Other immune mediators, such as leukotrienes and prostaglandins, are also implicated as they act on blood vessels to cause nasal congestion. Four to six hours after the initial response, an influx of cytokines, such as interleukins (IL)-4 and IL-13, from mast cells occurs, signifying the development of the late-phase response. These cytokines, in turn, facilitate the infiltration of eosinophils, T-lymphocytes, and basophils into the nasal mucosa and produce nasal edema with resultant congestion.
Epidemiology of Allergic Rhinitis
The prevalence of allergic rhinitis based on physician diagnosis is approximately 15%; however, the prevalence is estimated to be as high as 30% based on patients with nasal symptoms. AR is known to peak in the second to fourth decades of life and then gradually decline. The incidence of AR in the pediatric population is also quite high, making it one of the most common chronic pediatric disorders. According to data from the International Study for Asthma and Allergies in Childhood, 14.6% in the 13 to 14 year age group and 8.5% in the 6 to 7 year age group display symptoms of rhinoconjunctivitis linked to allergic rhinitis. Seasonal allergic rhinitis seems to be more common in the pediatric age group, whereas chronic rhinitis is more prevalent in adults.
Symptoms and Causes
Allergic rhinitis can appear throughout the year. Outdoor allergies are worse in the spring, summer, and early fall. In warm weather, weeds and flowers bloom, and pollen counts are higher. Indoor allergies, such as those from pets and dust mites, can get worse in winter because people spend more time indoors with their windows closed.
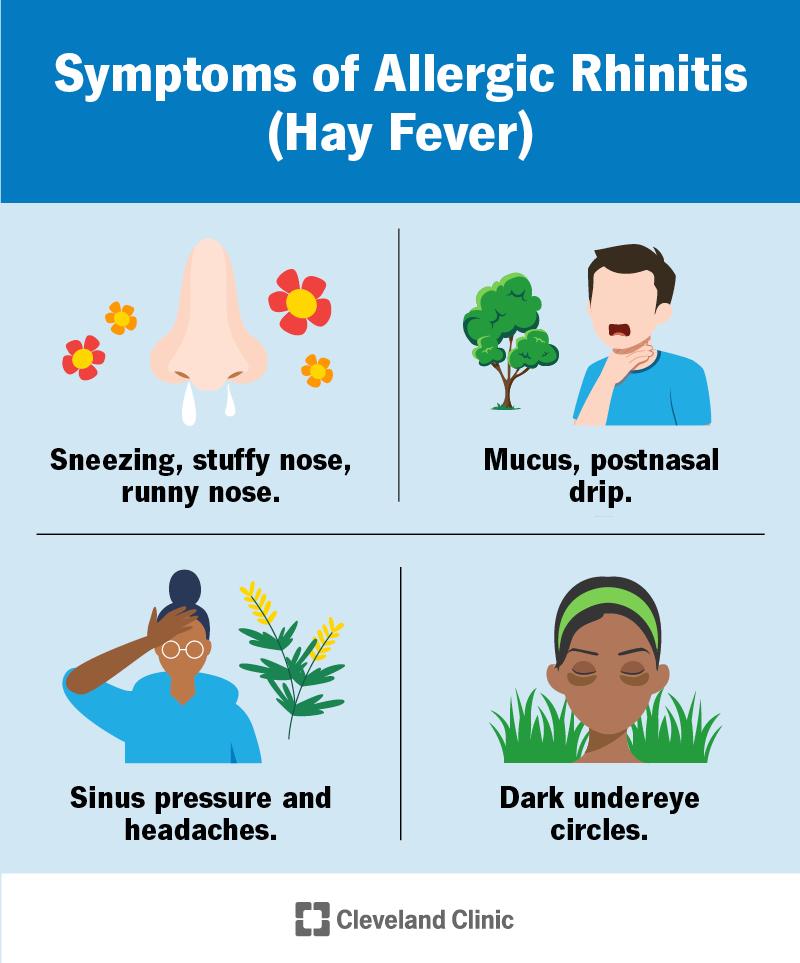
Symptoms of allergic rhinitis include:
- Nasal stuffiness (congestion), sneezing and runny nose
- Itchy nose, throat and eyes
- Watery, itchy, red eyes
- Headaches, sinus pressure and dark circles under the eyes
- More mucus in the nose and throat
- Extreme tiredness and fatigue, often due to poor sleep
- Sore throat from mucus dripping down the throat
- Cough
- Wheezing, coughing, and trouble breathing
- Swollen, bruised-appearing skin under the eyes, known as allergic shiners
There’s no way to prevent allergic rhinitis completely, but lifestyle changes can help to live with allergic. To reduce symptoms, the activity people should do:
Allergic rhinitis can be treat in several ways, these include medications:
a. Anhistamines
Antihistamine medications are available with a prescription or over the counter (OTC). Antihistamines work by blocking the histamine that the body releases during an allergic response. Antihistamines come as pills, liquids, eye drops, nasal sprays and inhalers. Some antihistamines include:
b. Decongestants
Decongestants can increase blood pressure and cause headaches, trouble sleeping and irritability. Nasal decongestants can be addictive when use for longer than five days. The decongestants include:
c. Eye Drops and Nasal Sprays
Eye drops and nasal sprays can help relieve itchiness and other allergy-related symptoms for a short time. However, depending on the product, avoid long-term use. Like decongestants, overusing certain eye drops and nose drops can also cause a rebound effect.
d. Corticosteroids
Antihistamines may be used in patients with mild symptoms or who do not want to use intranasal corticosteroids (INCS). For those with persistent or moderate to severe symptoms, INCS is recommended. Fixed combinations of INCS and antihistamines are mainly used in patients who do not benefit from INCS alone.
e. Immunotherapy
The doctor may recommend immunotherapy or allergy shots if patient have severe allergies. The patient can use this treatment plan in conjunction with medications to control symptoms. These shots decrease the immune response to particular allergens over time and require a long-term commitment to a treatment plan.
An allergy shot regimen begins with a buildup phase. During this phase, patient will go to a doctor for a shot one to three times per week for about three to six months to let the body get used to the allergen in the shot. During the maintenance phase, the patient will likely need to see doctor for shots every two to four weeks over the course of three to five years.
RHINOMAX® is a solution for allergic rhinitis. RHINOMAX® is a combination of Pseudoephedrine Sulphate as decongestant and Desloratadine 2,5 mg as antihistamine. RHINOMAX® as modified release tablet has a unique properties like long acting therapy, fast onset, and no sedative effect. The modified release tablet in RHINOMAX® dosage form making the medicine has a long acting effect, so the patients can take RHINOMAX® in the morning or afternoon, and unlike the other antihistamine medicine, consumption RHINOMAX® will not make the patients sleepy.
Reference
Fauzi, Sudiro M., Lestari BW. 2015. Prevalence of Allergic Rhinitis based on World Health Organization (ARIA-WHO) questionnaire among Batch 2010 Students of the Faculty of Medicine Universitas Padjadjaran. AMJ.2015;2(4):620-5
Afriana A., Syabriansyah., Dita DAA. 2023. Profile of Allergic Rhinitis and its Association with Chronic Suppurative Otitis Media. Muhammadiyah Medical Journal Vol. 4., No.2, Year 2023.
Liu, Y., Liu, Z. 2022. Epidemiology, Prevention and Clinical Treatment of Allergic Rhinitis: More Understanding, Better Patient Care. J. Clin. Med. 2022, 11, 6062.
Sharma K., Akre S., Chakole S., Wanjari MB. 2022. Allergic Rhinitis and Treatment Modalities: A Review of Literature. Cureus 14(8): e28501.
https://my.clevelandclinic.org/health/diseases/8622-allergic-rhinitis-hay-fever
https://www.ncbi.nlm.nih.gov/books/NBK538186/
https://www.healthline.com/health/allergic-rhinitis#treatments